
Applications for the LAMP Fellowship 2025-26 will open soon. Sign up here to be notified when the dates are announced.
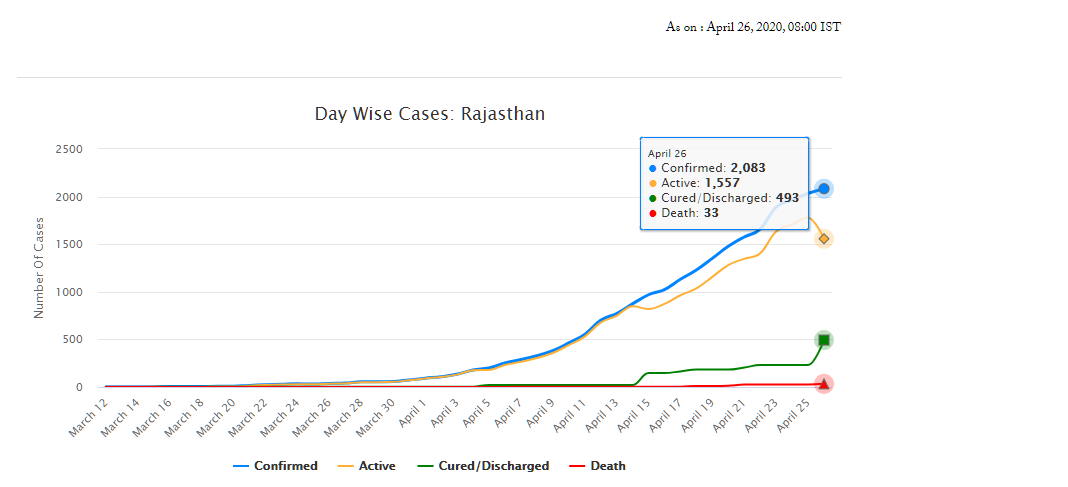
As of April 26, Rajasthan has 2,083 confirmed cases of COVID-19 (fifth highest in the country), of which 493 have recovered and 33 have died. On March 18, the Rajasthan government had declared a state-wide curfew till March 31, to check the spread of the disease. A nation-wide lockdown has also been in place since March 25 and is currently, extended up to May 3. The state has announced several policy decisions to prevent the spread of the virus and provide relief for those affected by it. This blog summarises the key policy measures taken by the Government of Rajasthan in response to the COVID-19 pandemic.
Early measures for containment
Between late January and early February, Rajasthan Government’s measures were aimed towards identification, screening and testing, and constant monitoring of passenger arrivals from China. Instructions were also issued to district health officials for various prevention, treatment, & control related activities, such as (i) mandatory 28-day home isolation for all travellers from China, (ii) running awareness campaigns, and (iii) ensuring adequate supplies of Personal Protection Equipments (PPEs). Some of the other measures, taken prior to the state-wide lockdown, are summarised below:
Administrative measures
The government announced the formation of Rapid Response Teams (RRTs), at the medical college-level and at district-level on March 3 and 5, respectively.
The District Collector was appointed as the Nodal Officer for all COVID-19 containment activities. Control Rooms were to be opened at all Sub-divisional offices. The concerned officers were also directed to strengthen information dissemination mechanisms and tackle the menace of fake news.
Directives were issued on March 11 to rural health workers/officials to report for duty on Gazetted holidays. Further, government departments were shut down between March 22 and March 31. Only essential departments such as Health Services were allowed to function on a rotation basis at 50% capacity and special / emergency leaves were permitted.
Travel and Movement
Air travellers were to undergo 14-day home isolation and were also required to provide an undertaking for the same. Besides, those violating the mandated isolation/quarantine were liable to be punished under Section. 188 of the Indian Penal Code. Penalties are imposed under this section on persons for the willful violation of orders that have been duly passed by a public servant.
All institutions and establishments, such as (i) educational institutions, theatres, and gyms, (ii) anganwadis, (iii) bars, discos, libraries, restaurants etc, (iv) museums and tourist places, were directed to be shut down till March 31.
The daily Jan Sunwai at the Chief Minister’s residence was cancelled until further notice. Various government offices were directed to shut down and exams of schools and colleges were postponed.
On March 24, the government issued a state-wide ban on the movement of private vehicles till March 31.
Health Measures
Advisories regarding prevention and control measures were issued to: (i) District Collectors, regarding sample collection and transportation, hotels, and preparedness of hospitals, (ii) Police department, to stop using breath analysers, (iii) Private hospitals, regarding preparedness and monitoring activities, and (iv) Temple trusts, to disinfect their premises with chemicals.
The government issued Standard Operating Procedures for conducting mock drills in emergency response handling of COVID-19 cases. Training and capacity building measures were also initiated for (i) Railways, Army personnel etc and (ii) ASHA workers, through video conferencing.
A model micro-plan for containing local transmission of COVID was released. Key features of the plan include: (i) identification and mapping of affected areas, (ii) activities for prevention control, surveillance, and contact tracing, (iii) human resource management, including roles and responsibilities, (iv) various infrastructural and logistical support, such as hospitals, labs etc, and (v) communication and data management.
Resource Management: Private hospitals and medical colleges were instructed to reserve 25 % of beds for COVID-19 patients. They were also instructed to utilise faculty from the departments of Preventive and Social Medicine to conduct health education and awareness activities.
Over 6000 Students of nursing schools were employed in assisting the health department to conduct screening activities being conducted at public places, railways stations, bus stands etc.
Further, the government issued guidelines to ensure the rational use of PPEs.
Welfare Measures
The government announced financial assistance, in the form of encouragement grants, to health professionals engaged in treating COVID-19 patients.
Steps were also taken by the government to ensure speedy disbursal of pensions for February and March.
The government also initiated the replacement of the biometric authentication with an OTP process for distribution of ration via the Public Distribution System (PDS).
During the lockdown
State-wide curfew announced on March 18 has been followed by a nation-wide lockdown between March 25 and May 3. However, certain relaxations have been recommended by the state government from April 21 onwards. Some of the key measures undertaken during the lockdown period are:
Administrative Measures
Advisory groups and task forces were set up on – (i) COVID-19 prevention, (ii) Health and Economy, and (iii) Higher education. These groups will provide advice on the way forward for (i) prevention and containment activities, (ii) post-lockdown strategies and strategies to revive the economy, and (iii) to address the challenges facing the higher education sector respectively.
Services of retiring medical and paramedical professionals retiring between March and August have been extended till September 2020.
Essential Goods and Services
A Drug Supply Control Room was set up at the Rajasthan Pharmacy Council. This is to ensure uninterrupted supply of medicines during the lockdown and will also assist in facilitating home delivery of medicines.
The government permitted Fair Price Shops to sell products such as masalas, sanitisers, and hygiene products, in addition to food grains.
Village service cooperatives were declared as secondary markets to facilitate farmers to sell their produce near their own fields/villages during the lockdown.
A Whatsapp helpline was also set up for complaints regarding hoarding, black marketing, and overpricing.
Travel and Movement
Once lockdown was in place, the government issued instructions to identify, screen, and categorise people from other states who have travelled to Rajasthan. They were to be categorised into: (i) people displaying symptoms to be put in isolation wards, (ii) people over 60 years of age with symptoms and co-morbidities to be put in quarantine centres, and (iii) asymptomatic people to be home quarantined.
On March 28, the government announced the availability of buses to transport people during the lockdown. Further, stranded students in Kota were allowed to return to their respective states.
On April 2, a portal and a helpline were launched to help stranded foreign tourists and NRIs.
On April 11, an e-pass facility was launched for movement of people and vehicles.
Health Measures
To identify COVID-19 patients, district officials were instructed to monitor people with ARI/URI/Pneumonia or other breathing difficulties coming into hospital OPDs. Pharmacists were also instructed to not issue medicines for cold/cough without prescriptions.
A mobile app – Raj COVID Info – was developed by the government for tracking of quarantined people. Quarantined persons are required to send their selfie clicks at regular intervals, failing which a notification would be sent by the app. The app also provides a lot of information on COVID-19, such as the number of cases, and press releases by the government.
Due to the lockdown, people had restricted access to hospitals and treatment. Thus, instructions were issued to utilise Mobile Medical Vans for treatment/screening and also as mobile OPDs.
On April 20, a detailed action plan for prevention and control of COVID-19 was released. The report recommended: (i) preparation of a containment plan, (ii) formation of RRTs, (iii) testing protocols, (iv) setting up of control room and helpline, (v) designated quarantine centres and COVID-19 hospitals, (vi) roles and responsibilities, and (vii) other logistics.
Welfare Measures
The government issued instructions to make medicines available free of cost to senior citizens and other patients with chronic illnesses through the Chief Minister’s Free Medicine Scheme.
Rs 60 crore was allotted to Panchayati Raj Institutions to purchase PPEs and for other prevention activities.
A one-time cash transfer of Rs 1000 to over 15 lakh construction workers was announced. Similar cash transfer of Rs 1000 was announced for poor people who were deprived of livelihood during the lockdown, particularly those people with no social security benefits. Eligible families would be selected through the Aadhaar database. Further, an additional cash transfer of Rs 1500 to needy eligible families from different categories was announced.
The state also announced an aid of Rs 50 lakh to the families of frontline workers who lose their lives due to COVID-19.
To maintain social distancing, the government will conduct a door-to-door distribution of ration to select beneficiaries in rural areas of the state. The government also announced the distribution of free wheat for April, May, and June, under the National Food Security Act, 2013. Ration will also be distributed to stranded migrant families from Pakistan, living in the state.
The government announced free tractor & farming equipment on rent in tie-up with farming equipment manufacturers to assist economically weak small & marginal farmers.
Other Measures
Education: Project SMILE was launched to connect students and teachers online during the lockdown. Study material would be sent through specially formed Whatsapp groups. For each subject, 30-40 minute content videos have been prepared by the Education Department.
Industry: On April 18, new guidelines were issued for industries and enterprises to resume operations from April 20 onwards. Industries located in rural areas or export units / SEZs in municipal areas where accommodation facilities for workers are present, are allowed to function. Factories have been permitted to increase the working hours from 8 hours to 12 hours per day, to reduce the requirement of workers in factories. This exemption has been allowed for the next three months for factories operating at 60% to 65% of manpower capacity.
For more information on the spread of COVID-19 and the central and state government response to the pandemic, please see here.
The National Medical Commission (NMC) Bill, 2017 was introduced in Lok Sabha in December, 2017. It was examined by the Standing Committee on Health, which submitted its report during Budget Session 2018. The Bill seeks to regulate medical education and practice in India. In this post, we analyse the Bill in its current form.
How is medical education and practice regulated currently?
The Medical Council of India (MCI) is responsible for regulating medical education and practice. Over the years, there have been several issues with the functioning of the MCI with respect to its regulatory role, composition, allegations of corruption, and lack of accountability. For example, MCI is an elected body where its members are elected by medical practitioners themselves, i.e. the regulator is elected by the regulated. In light of such issues, experts recommended nomination based constitution of the MCI instead of election, and separating the regulation of medical education and medical practice. They suggested that legislative changes should be brought in to overhaul the functioning of the MCI.
To meet this objective, the Bill repeals the Indian Medical Council Act, 1956 and dissolves the current Medical Council of India (MCI) which regulates medical education and practice.
Who will be a part of the NMC?
The NMC will consist of 25 members, of which at least 17 (68%) will be medical practitioners. The Standing Committee has noted that the current MCI is non-diverse and consists mostly of doctors who look out for their own self-interest over larger public interest. In order to reduce the monopoly of doctors, it recommended that the MCI should include diverse stakeholders such as public health experts, social scientists, and health economists. In other countries, such as the United Kingdom, the General Medical Council (GMC) responsible for regulating medical education and practice consists of 12 medical practitioners and 12 lay members (such as community health members, and administrators from the local government).
How will the issues of medical misconduct be addressed?
The State Medical Council will receive complaints relating to professional or ethical misconduct against a registered doctor. If the doctor is aggrieved by the decision of the State Medical Council, he may appeal to the Ethics and Medical Registration Board, and further before the NMC. Appeals against the decision of the NMC will lie before the central government. It is unclear why the central government is an appellate authority with regard to such matters.
It may be argued that disputes related to ethics and misconduct in medical practice may require judicial expertise. For example, in the UK, the GMC receives complaints with regard to ethical misconduct and is required to do an initial documentary investigation. It then forwards the complaint to a Tribunal, which is a judicial body independent of the GMC. The adjudication and final disciplinary action is decided by the Tribunal.
What will the NMC’s role be in fee regulation of private medical colleges?
In India, the Supreme Court has held that private providers of education have to operate as charitable and not for profit institutions. Despite this, many private education institutions continue to charge exorbitant fees which makes medical education unaffordable and inaccessible to meritorious students. Currently, for private unaided medical colleges, the fee structure is decided by a committee set up by state governments under the chairmanship of a retired High Court judge. The Bill allows the NMC to frame guidelines for determination of fees for up to 40% of seats in private medical colleges and deemed universities. The question is whether the NMC as a regulator should regulate fees charged by private medical colleges.
A NITI Aayog Committee (2016) was of the opinion that a fee cap would discourage the entry of private colleges, therefore, limiting the expansion of medical education. It also observed that it is difficult to enforce such a fee cap and could lead medical colleges to continue charging high fees under other pretexts.
Note that the Parliamentary Standing Committee (2018) which examined the Bill has recommended continuing the current system of fee structures being decided by the Committee under the chairmanship of a retired High Court judge. However, for those private medical colleges and deemed universities, unregulated under the existing mechanism, fee must be regulated for at least 50% of the seats. The Union Cabinet has approved an Amendment to increase the regulation of fees to 50% of seats.
How will doctors become eligible to practice?
The Bill introduces a National Licentiate Examination for students graduating from medical institutions in order to obtain a licence to practice as a medical professional.
However, the NMC may permit a medical practitioner to perform surgery or practice medicine without qualifying the National Licentiate Examination, in such circumstances and for such period as may be specified by regulations. The Ministry of Health and Family Welfare has clarified that this exemption is not meant to allow doctors failing the National Licentiate Examination to practice but is intended to allow medical professionals like nurse practitioners and dentists to practice. It is unclear from the Bill that the term ‘medical practitioner’ includes medical professionals (like nurses) other than MBBS doctors.
Further, the Bill does not specify the validity period of this licence to practice. In other countries such as the United Kingdom and Australia, a licence to practice needs to be periodically renewed. For example, in the UK the licence has to be renewed every five years, and in Australia it has to renewed annually.
What are the issues around the bridge course for AYUSH practitioners to prescribe modern medicine?
The debate around AYUSH practitioners prescribing modern medicine
There is a provision in the Bill which states that there may be a bridge course which AYUSH practitioners (practicing Ayurveda, Yoga and Naturopathy, Unani, Siddha and Homoeopathy) can undertake in order to prescribe certain kinds of modern medicine. There are differing views on whether AYUSH practitioners should prescribe modern medicines.
Over the years, various committees have recommended a functional integration among various systems of medicine i.e. Ayurveda, modern medicine, and others. On the other hand, experts state that the bridge course may promote the positioning of AYUSH practitioners as stand-ins for allopathic doctors owing to the shortage of doctors across the country. This in turn may affect the development of AYUSH systems of medicine as independent systems of medicine.
Moreover, AYUSH doctors do not have to go through any licentiate examination to be registered by the NMC, unlike the other doctors. Recently, the Union Cabinet has approved an Amendment to remove the provision of the bridge course.
Status of other kinds of medical personnel
As of January 2018, the doctor to population ratio in India was 1:1655 compared to the World Health Organisation standard of 1:1000. The Ministry of Health and Family Welfare stated that the introduction of the bridge course for AYUSH practitioners under the Bill will help fill in the gaps of availability of medical professionals.
If the purpose of the bridge course is to address shortage of medical professionals, it is unclear why the option to take the bridge course does not apply to other cadres of allopathic medical professionals such as nurses, and dentists. There are other countries where medical professionals other than doctors are allowed to prescribe allopathic medicine. For example, Nurse Practitioners in the USA provide a full range of primary, acute, and specialty health care services, including ordering and performing diagnostic tests, and prescribing medications. For this purpose, Nurse Practitioners must complete a master’s or doctoral degree program, advanced clinical training, and obtain a national certification.